The Importance of Blood Pressure Measurement
The importance of accurate blood pressure determinations cannot be overemphasized. To obtain accurate blood pressure readings, the user requires 1) An accurate pressure measuring instrument, 2) The correct size cuff as it relates to the circumference of the limb and 3) Good measurement technique.
Blood pressure is a very important vital sign; if it is high it can lead to many negative health effects including heart attack, stroke and kidney failure. About 20% of the people in the U.S. are hypertensive; many of them do not know it because there are no symptoms to identify it. Accurate blood pressure readings are critically important since erroneous readings can lead to misdiagnosis and ultimately result in treatment errors.
Accurate measurement of blood pressure relies, as it always has, on the use of a correct size cuff, good measurement technique and an instrument of known accuracy, dependability and reproducibility. We have been providing such instruments since 1916.
How is blood pressure measured?
TECHNIQUE OF MEASUREMENT
“In the everyday practice of medicine, a combination of the palpatory and auscultatory methods is used”.
1 – Application of the compression cuff
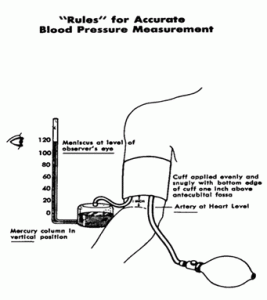
The blood pressure is generally recorded in the arm with the patient in a sitting or recumbent position. The physician should arrange his desk and chair or examining table so the patient’s right arm is always and inevitably presented for recording of the blood pressure. The arm should be abducted, slightly flexed, and supported by a smooth, firm surface. The artery over which the blood pressure is to be recorded should be at a level with the heart. It is not necessary for the manometer to be at heart level.
The deflated compression cuff is applied evenly and snugly, but without constriction, around the right arm. The lower edge of the cuff should be 2.5 cm above the point at which the receiver of the stethoscope is to be placed.
2 – Palpatory Method
The radial or popliteal pulse is palpated and the rate and rhythm are noted. The compression cuff is then inflated to about 30 mm Hg above the pressure at which the radial pulse disappears. (When the cuff is inflated, it should not bulge nor become displaced.) The cuff is then deflated at a rate of 2 to 3 mm Hg per heartbeat. The level of pressure at which the pulse in the radial artery returns is noted and recorded as the systolic arterial blood pressure. The diastolic blood pressure is difficult to measure by palpation and is not generally determined by this method.
3 – Auscultatory Method
After the systolic blood pressure has been determined by the palpatory method, the blood pressure is then determined by auscultation over the artery at a point below the compression cuff, which has remained on the arm. The artery is first palpated, and then the receiver of the stethoscope is applied lightly but snugly over it to produce an airtight seal. The receiver must not come into contact with the patient’s clothing nor with the compression cuff. The compression cuff is then inflated rapidly to about 30 mm Hg above the systolic pressure as previously determined by the palpatory method. The cuff is then deflated at a rate of 2 to 3 mm Hg per heartbeat. While the physician is watching the meniscus of the mercury column (or the aneroid pointer), the pressure at which characteristic changes in the Korotkoff sounds occur is noted. From the changes in the quality of these sounds, the systolic and diastolic blood pressure are determined.
The systolic blood pressure
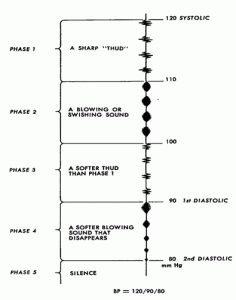
The pressure within the compression cuff indicated by the level of the mercury column (or the aneroid pointer), at the moment the Korotkoff sounds are first heard, represents the systolic blood pressure. This is the start of Phase 1 (Fig. 3) which begins with faint, clear and rhythmic tapping or thumping sounds that gradually increase in intensity.
The diastolic blood pressure
The pressure within the compression cuff indicated by the level of the mercury column (or the aneroid pointer), at the moment the sound suddenly becomes muffled, represents the first diastolic pressure (beginning of Phase 4). The second diastolic pressure is the pressure within the compression cuff at the moment the sounds finally disappear (beginning of Phase 5).
“Some physicians consider the diastolic pressure to be equal to the pressure in the compression cuff at the moment the first sound of Phase 4 is heard. This has been found to be somewhat higher than the pressure recorded directly and simultaneously… Until more is known, it is advisable to record two diastolic pressures; the first at the onset of Phase 4 and the second upon the development of faint sounds in Phase 4 or at the moment of disappearance of the Korotkoff sounds. With experience and clinical judgment, serious errors in measuring diastolic blood pressure can usually be avoided.”
SUMMARY
Steps in taking blood pressure
1 – Snug application of compression cuff.
2 – Palpation of radial artery as compression cuff is inflated.
3 – Palpation of radial artery as cuff is deflated at 2 to 3 mm Hg per heartbeat.
4 – Careful placement of stethoscope receiver.
5 – Inflation of compression cuff above systolic pressure.
6 – Deflation of the cuff at a rate of 2 to 3 mm Hg per heartbeat to determine systolic and diastolic blood pressure.
“Regardless of the mechanism responsible for the production of the Korotkoff sounds and the pros and cons for employing the beginning of Phase 4 or of Phase 5 to measure diastolic pressure, the auscultatory method for obtaining arterial blood pressure is the clinical method par excellence. The wise, careful, and thoughtful physician will not make serious clinical errors in diagnosis and treatment if the uses the ausclultatory method properly.”
What is blood pressure?
Arterial blood pressure is the force exerted by the blood on an area of the wall of an artery as it is pushed through the circulatory system. During the course of the cardiac cycle, the arterial blood pressure is constantly changing . As the heart beats, the highest pressure in this cycle (systolic blood pressure) is recorded. Between beats, the lowest pressure (diastolic blood pressure) is recorded. The systolic number is always stated first and the diastolic number is listed second.
For example: 122/76 (122 over 76); systolic = 122, diastolic = 76.
Blood pressure is determined by a number of factors including:
- Cardiac output
- Peripheral vascular resistance
- Volume of blood in the arterial system
- Viscosity (density) of the blood
Elasticity of the arterial walls
The exact contribution of each factor is not known, but peripheral resistance and cardiac output have the greatest influence on blood pressure.
How can I tell if I have high blood pressure?
The only way to find out if you have high blood pressure is to have your blood pressure checked. Your doctor or other qualified health professional should check your blood pressure at least once every two years. Should your blood pressure reading be elevated, you don’t necessarily have high blood pressure. However further observation is recommended.
What is hypertension?
Hypertension does not refer to being tense, nervous or hyperactive. It is simply the medical term for high blood pressure. Because high blood pressure usually has no symptoms, many people have high blood pressure for years without knowing it. That’s why it’s so dangerous.
What about low blood pressure?
Generally speaking, the lower your blood pressure reading is, the better. However, unusually low readings should be evaluated for clinical significance. Examples include certain nerve disorders, endocrine disorders, prolonged bed rest decreases in blood volume due to severe bleeding (hemorrhage) or dehydration. Usually, people with dangerously low blood pressure exhibit symptoms such as lightheadedness or fainting.
What kinds of manometers are available?
There are three types of blood pressure apparatus: the mercury-gravity manometer, the aneroid gauge and electronic devices.
The mercury-gravity manometer consists of a calibrated glass tube with a reservoir containing mercury. The reservoir communicates with the compression cuff through a rubber tube. When pressure is exerted by inflating the cuff the mercury rises in the glass tube.
“Once the mercury manometer is calibrated, recalibration is unnecessary. The mercury manometer is the most reliable recorder available for the clinical measurement of blood pressure.” (Pg. 49-50 Primer of Clinical Measurement of Blood Pressure, BURCH and DePASQUALE, Tulane University Medical School.)
The aneroid gauge consists of a metal bellows and a watch-like movement connected to the compression cuff. Variations of pressure within the system cause the bellows to expand and contract. Movement of the bellows rotates a gear that turns a pointer pivoted on bearings, across a calibrated dial.
Obviously the adjustment of the mechanical system of the aneroid gauge is more easily disturbed than that of a mercury manometer. For this reason, the aneroid gauge must be calibrated against a mercury manometer at regular intervals. Since the blood pressure recorded with the aneroid gauge depends upon the elasticity of the metal bellows, it is subject to errors inherent in the elastic properties of metal such as ‘seasoning’, hysteresis and drift. Remember, the mere fact that the pointer indicates zero on the dial of the aneroid gauge is no guarantee of accuracy over the whole pressure range.
The electronic device operates on the extrapolation of deflections of a transducer coupled with an algorithmic derivation of a selected oscillation. It does not use the auscultation of Korotkoff sounds.



